
The consequences of the global coronavirus for mental health have been dire, particularly for adolescents and young adults, who have faced large disruptions to their education and living situations and may suffer lifelong economic impacts.
To examine how the pandemic has affected their daily lifestyle and well-being, we take advantage of an ongoing wellness study in which 682 US college students received wearable devices (Fitbits) and answer repeated surveys about their time use and mental health over the course of a semester. The study allows us to compare participants before and during the pandemic (Figure 1).
In March 2020, when classes moved online and shutdowns began, the average number of steps participants achieved declined from about 10,000 to 4,600 per day, a decrease of over 50%. Daily minutes of physical activity declined by about a third, and sleep increased by about 25–30 minutes per night due primarily to students waking up later. Time spent socializing declined by over half to less than 30 minutes per day; screen time more than doubled to over five hours per day.
These lifestyle disruptions occurred alongside stark declines in mental health. Based on the Center for Epidemiologic Studies Depression Scale (CES-D), Figure 2 reports average CES-D scores by semester. The frequency of symptoms of depression, such as helplessness or loneliness, increased by over 60% at the onset of the pandemic. Participants with a CES-D score of 16 or above are considered at risk for clinical depression. As of April 2020, 61% of participants were estimated to be at risk, a 90% increase compared to the same population before the pandemic.
Combining our measures of lifestyle disruption and mental health, disruptions to physical activity emerge as a leading risk factor for depression during the pandemic. Importantly, those who maintained their habits were at significantly lower risk than those who experienced large average declines in physical activity.
Building on these findings, we implemented an experiment in which we randomized half our participants to receive incentives for walking at least 10,000 steps per day for two weeks. Our intervention significantly increased daily steps, with the incentivized group close to their baseline pre-pandemic levels. The impact on physical activity did not, however, translate into an improvement in mental health. Taken together, our findings suggest a puzzle: disruptions to physical activity and mental health are strongly associated, but restoring physical activity is not meaningfully linked to restoring mental health.
We need to know the effectiveness of longer interventions or attempt to restore physical health along with other important lifestyle habits, such as social interactions. Also important is knowing which interventions will improve resilience in the face of the large disruptions caused by the pandemic.
Figure 1. Average daily steps before and during Covid-19
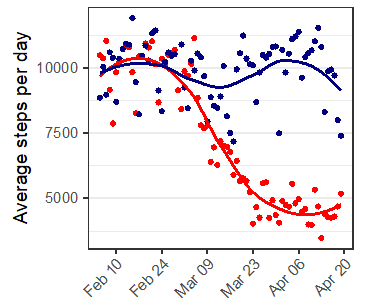
Note: Spring 2019 (blue) and Spring 2020 (red) semesters.
Figure 2. Students’ CES-D depression before and during Covid-19
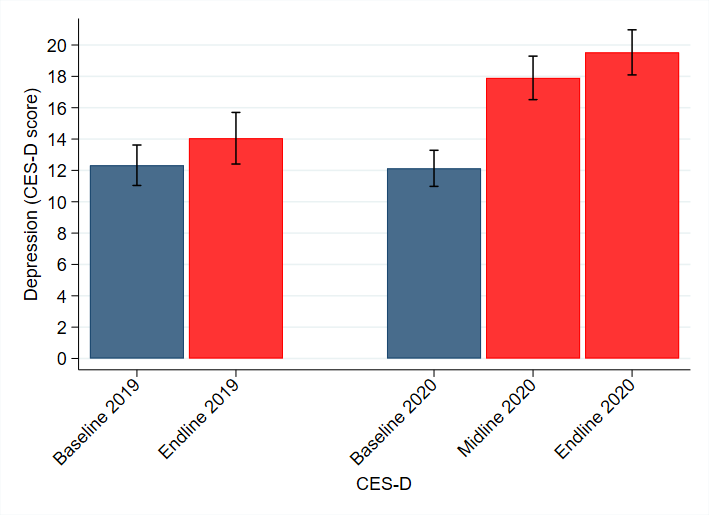
Note: (CES-D) score, beginning (February) and end (April) of semester Spring 2019 and Spring 2020, middle (March 2020 only). Bars indicate 95% confidence intervals.
© Osea Giuntella, Kelly Hyde, Silvia Saccardo, and Sally Sadoff
Osea Giuntella is assistant professor of economics at the University of Pittsburgh, USA, and an IZA Research Fellow.
Kelly Hyde is an economics PhD student at the University of Pittsburgh, USA.
Silvia Saccardo is assistant professor in the Department of Social and Decision Sciences at Carnegie Mellon University, USA, and a CESifo Research Network Affiliate.
Sally Sadoff is associate professor of economics and strategic management in the Rady School of Management at the University of California, San Diego, USA.
Find more IZA World of Labor coronavirus content on our curated topics pages: National responses to Covid-19 and Covid-19—Pandemics and the labor market.
Please note:
We recognize that IZA World of Labor articles may prompt discussion and possibly controversy. Opinion pieces, such as the one above, capture ideas and debates concisely, and anchor them with real-world examples. Opinions stated here do not necessarily reflect those of the IZA.