Elevator pitch
Upon arrival in a host country, immigrants often have lower obesity rates (as measured for instance by BMI—body mass index) than their native counterparts do, but these rates converge over time. In light of the worldwide obesity epidemic and the flow of immigrants into host countries with higher obesity rates, it is important to understand the consequences of such assimilation. Policymakers could benefit from a discussion of the impact of immigrant obesity on labor market outcomes and the use of public services. In particular, policies could find ways to improve immigrants’ access to health care for both the prevention and treatment of obesity.
Key findings
Pros
Immigrants arrive with lower BMI and lower obesity rates than those of natives.
Obesity among immigrants remains low in ethnically concentrated areas where acculturation occurs slowly.
Immigrant obesity remains low for males and the college-educated.
In the US there is little evidence of a wage effect of obesity for immigrant men.
Immigrants rarely seek health-care services, so increases in obesity should not result in the overuse of public services.
Cons
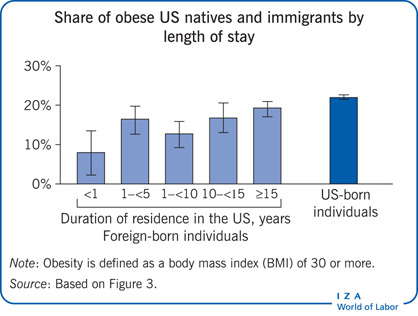
Migration generally flows from low- to high-BMI countries. As migrants’ stays increase, they adopt natives’ unhealthy lifestyles and their BMIs approach the higher levels of native populations.
In the UK, lower immigrant obesity rates are associated with higher wages and employment.
In the US, obese immigrant women who stay less than five years incur a wage penalty; In the UK, obese immigrant men experience a significant wage penalty.
The children and grandchildren of immigrants face accelerated obesity rates.
Estimates of “healthy immigrant effects” and the labor market effects of weight may not fully account for factors that can bias the results.